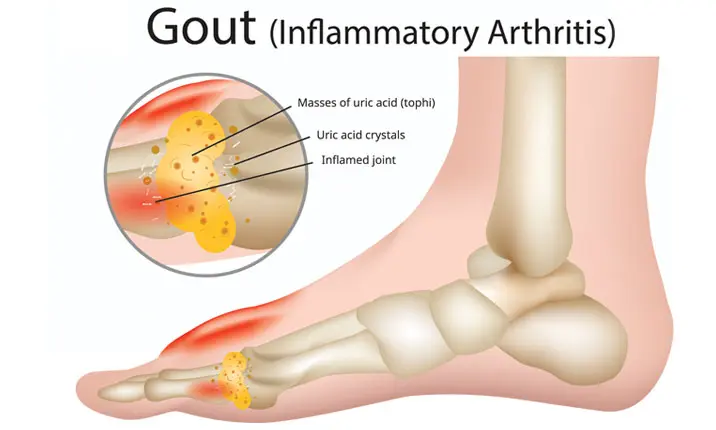
What is gout?
Gout is a form of arthritis that affects around 1% of the population and 6 times more men than women. It is caused by a build-up of uric acid crystals in the joints as a result of having too much uric acid in the body.
What causes uric acid build-up?
The body produces uric acid from purines (naturally occurring chemical compounds in food) when it breaks down the food you digest. This uric acid normally dissolves in the blood but if your body produces too much (10% of cases) or the kidneys excrete too little to eliminate it from the body (90% of cases), uric acid can build up over time and cause gout.
Gout symptoms occur when the body’s natural defence mechanisms attack the uric acid crystals in the joint fluid, which causes a release of inflammatory chemicals (cytokines), which cause heat, redness, swelling and pain around the joint. This cycle also sends more white blood cells to the joint, which accelerates the inflammatory process.
Am I at risk for gout?
The risk of developing gout is higher if someone in your family has a history of gout, but the following factors also play a part:
- Diet. Eating meat and seafood and taking drinks sweetened with fructose increase levels of uric acid as does alcohol consumption, especially of beer.
- Weight. The body produces more uric acid, which the kidneys have trouble eliminating when overweight.
- Existing chronic diseases. Untreated high blood pressure and chronic conditions such as heart and kidney diseases, diabetes and metabolic syndrome increase your risk of developing gout.
- Certain medications. Thiazide diuretics, commonly used to treat hypertension, and low-dose aspirin can increase uric acid levels, as can anti-rejection drugs prescribed after an organ transplant.
- Age and sex. Women before menopause produce less uric acid than men so are less likely than men to develop gout. However, their risk increases after menopause as uric acid levels rise. Men tend to develop gout between the ages of 30 – 50.
- Recent surgery or trauma. This tends to increase the risk of developing gout.
- Chemotherapy. This treatment kills tumour cells but the breakdown of purines from the cells can trigger a gout attack.
How do I know if I have gout?
Speak to a doctor to get an accurate diagnosis if there is pain, inflammation and swelling in any joint. The most common joint affected by gout is the big toe, although it can occur in the ankle, midfoot, knee and elbow. In a gout attack, you may also experience fever and chills, fatigue and malaise. If untreated, an attack may take weeks to resolve, but because gout is very painful and can restrict walking and mobility, patients generally seek medical help. Your doctor will be able to assess whether you are suffering from gout or another type of arthritis, and manage the condition accordingly.
Can gout be treated?
Gout should not be ignored as it is a progressive condition that is treatable in earlier stages. While treatment for gout is highly effective, the medication and lifestyle changes needed will be lifelong. If left untreated, over time, gout can cause irreparable damage to your joints.
Your doctor will take two approaches to treat and manage your condition:
Treat the current gout attack. Your doctor will prescribe anti-inflammatory medication of steroid injections and advise you to stay off your feet when your joint is inflamed. Your condition will clear up faster the sooner you get treatment. It is best to seek treatment within the first 24 hours of an attack.
Minimise the risk of future attacks from happening. To prevent future attacks, you need to control the amount of uric acid in your body. Your doctor will help with a plan for you to make lifestyle improvements such as removing trigger foods and beverages from your diet, taking more exercise and losing excess weight. However, for patients with high levels of uric acid, these lifestyle modifications won’t be enough and your doctor will prescribe you medications depending on the stage of disease and cause of gout to either:
- decrease the production of uric acid
- increase your excretion of uric acid
- increase your body’s ability to break down uric acid and/or
- reduce the ability of the uric acid crystals to cause inflammation.
Should I consider surgery for gout?
If you seek treatment early, your doctor and you should be able to manage your condition with medication and lifestyle changes to stop it advancing.
When left untreated or not properly managed, gout will progress to a stage known as chronic tophaceous gout within 10 years, which can be very disabling.
At this stage, hard deposits of uric acid, called tophi, form in and around the joints and may cause irreparable damage. At this point, your doctor will recommend one of the following 4 possible procedures. Depending on the damage, surgical costs can vary widely, depending on the type of surgery and which joint needs to be repaired.
Arthroscopic gout removal.
In less extreme cases, arthroscopic surgery may be used to remove uric acid in the joints, providing pain relief. This minimally-invasive technique has been found to have better functional outcomes than patients who were solely treated with medication.
Full recovery takes several weeks, with the small puncture wounds taking several days to heal, after which it is possible to resume normal daily activities. Active individuals should wait a few weeks to resume athletic activities.
Tophi removal surgery.
Tophi can get very painful and inflamed. They can even break through the skin, heightening the risk of bacterial infection. The crystals can track down to the bone. Removal of this much tissue will make the surgical wound very difficult to heal and a skin graft may be required. For this reason, your doctor will try to manage your condition aggressively with medication to trigger the tophi to reabsorb without the need for surgery.
The recovery time for tophi removal surgery can vary depending on several factors, including the size and number of tophi removed and the patient's overall health. In general, it may take several weeks to a few months to fully recover from tophi removal surgery.
Joint fusion surgery.
If the joint is permanently damaged, this surgery fuses smaller joints to increase joint stability and relieve pain. After surgery, it is normal to feel some pain and stiffness in the joint, and you will lose some range of motion. Overall, recovery can take up to 12 weeks, and physical therapy can help keep your other joints in good working shape.
Joint replacement surgery.
If the gout-infected joint is the knee, you will be a suitable candidate for knee replacement surgery, where an artificial joint replaces your diseased one. Joint replacement is considered a major surgery and would incur the most cost, relative to other forms of surgery.
Recovery from joint surgery can take around 6 weeks or more. You should expect to be homebound for the first 2 – 3 weeks, during which you will need help with your daily care. This is followed by several weeks of rehabilitation to regain your muscle strength, range of motion and mobility.
To manage your gout and avoid surgery, take your medications as prescribed and discuss any side effects with your doctor so that they can be managed. The medications available today have been successful at treating gout. However, if you think you need surgery, consult an orthopaedic surgeon to have your condition assessed.