What is eczema?
Eczema, commonly referred to as atopic dermatitis, causes patches of your skin to be itchy and inflamed.
Eczema is a long-lasting (chronic) condition that tends to flare up periodically. People who suffer from asthma, allergic rhinitis, or have relatives who have eczema, are at a higher risk of having the skin condition. Eczema is not contagious.
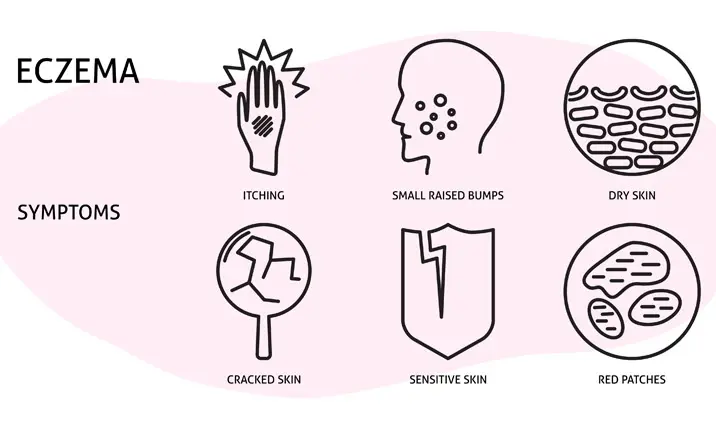
Symptoms of eczema
Symptoms of eczema may vary from person to person. Some of the most common symptoms of eczema include:
- Dry skin
- Patches on the skin that appear darker than the surrounding area
- Inflamed red rashes
- Skin that is thickened or leathery and cracked
- Itchiness that may become more severe at night
- Hard bumps on the skin that may leak fluid and form crusts when scratched
- Raw and sensitive skin as a result of scratching
Eczema symptoms can start in infancy and continue through adulthood. However, nearly half of children diagnosed with eczema will outgrow the condition or have their symptoms greatly improve by the time they reach puberty.
In other people it can start in the teenage years and disappear by young adulthood.
For many others, eczema can be a lifelong condition. There also be times when symptoms disappear (called the remission period) and other times when symptoms worsen (called flare-ups).
Types of eczema
When most people refer to eczema, they usually mean atopic dermatitis as it is the most common and chronic type of eczema. The following are other common types of eczema which may match your particular symptoms:
Contact dermatitis
This skin condition occurs when your skin comes into contact with irritants or allergic substances, leading to itchy red rashes or even blisters. The inflammation usually goes away following treatment and when the offending substance is removed.
Discoid/nummular dermatitis
This type of eczema causes round red patches on the skin and usually affects your legs. It can be mistaken as fungal infection.
Dyshidrotic dermatitis
Dyshidrotic eczema, also known as dyshidrotic dermatitis or pompholyx cause tiny blisters on the hands, fingers and soles of the feet. It is often seen in adults under 40 years although it can happen at any age.
Symptoms of dyshidrotic eczema usually starts as severe itching and burning of the skin on the hands and fingers. This further develops into tiny itchy blisters on the palms and sides of the fingers that may weep fluid.
Seborrheic dermatitis
Seborrheic dermatitis causes itchy, red, scaly rashes over oily skin areas of your scalp, eyebrows, eyelids, the sides of your nose, and behind your ears.
Causes of eczema
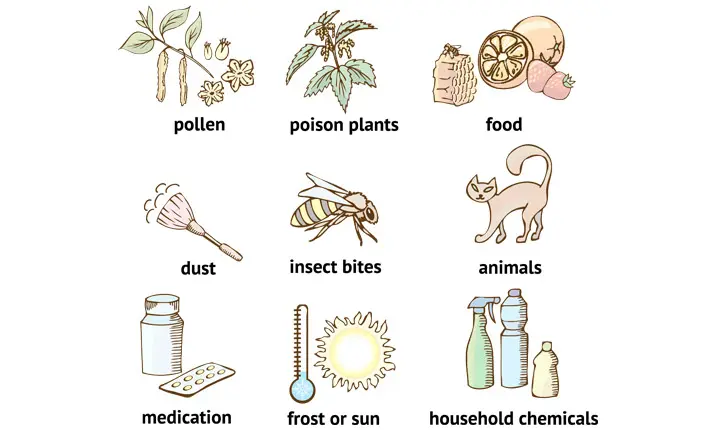
The cause of eczema is not fully understood but is believed to be a combination of dysfunctional skin barrier and an overactive immune system which may respond aggressively when exposed to irritants. Eczema triggers include:
- animal dander
- any infections eg. common colds, upper respiratory tract infections
- insect bites
- certain foods that may aggravate eczema in some patients
- chemicals found in cleaners and detergents that dry out the skin
- contact allergy eg. nickel, hair dye
- rough scratchy material, like wool
- stress
- sweating
- synthetic fabrics
- temperature changes, especially to heat
Managing eczema
Although living with eczema can sometimes be challenging, there are steps you can take to help better manage your eczema:
Skin care
- When bathing, use a mild soap or soap substitute that won't dry your skin, and afterwards apply a good moisturiser.
- Keep your skin moisturised throughout the day. Apply moisturiser daily and regularly to repair the skin barrier.
- Avoid taking very hot or very long showers as this can dry out your skin.
Don't scratch your eczematous skins
If you need some help controlling your eczema itch, you may want to consider antihistamines. Examples of antihistamines for eczema include:
- Cetirizine
- Loratadine
- Levocetirizine
- Desloratadine
- Fexofenadine
Treat skin inflammation with topical steroid creams
Different potency steroid creams can be used to treat eczema skin inflammation, depending on extent and area of rashes. Your doctor can explain the proper use of creams and monitor for side effects. There are also non-steroid creams to treat skin inflammation, generally used for sensitive areas on the face and eyelids.
Treatment for flare-ups
If you have a bad flare, you may require intensive topical treatment (wet wraps) or a course of oral steroids. Oral medications may be required to treat any skin infections or infected eczema.
Treatment for difficult-to-control eczema
If flare-ups are recurrent or eczema is difficult to control, you may need to escalate treatment. Your doctor may prescribe medication to control the immune system (eg. ciclosporin, azathioprine, or the new biologic injection dupilumab). Phototherapy may be another option.
Allergy tests (prick or patch test)
Allergy tests may be required for certain types of eczema and to identify potential substances which your skin may be allergic to.
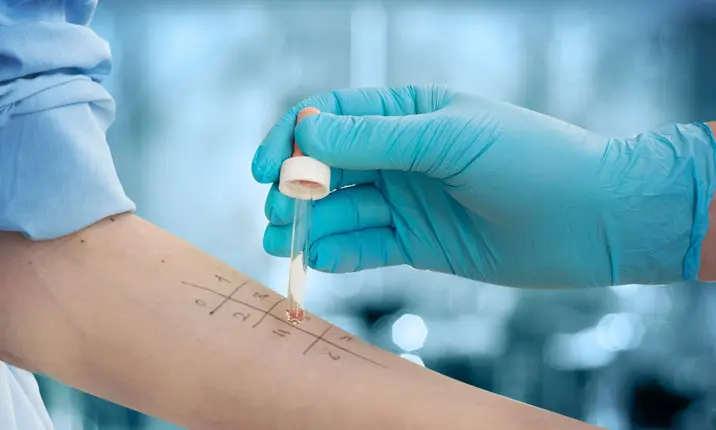
Skin prick test
A skin prick test can test for as many as 50 different substances at once such as, pollen, mold, pet dander, dust mites and food. The test is performed by gently pricking the skin's surface using needles and placing small drops of allergen extracts into the skin's surface. If you are allergic to any of the tested substances, a raised, red, itchy bump will appear.
Patch test
Patch tests are done to see if a particular substance is causing an allergic skin inflammation. Substances that are tested may include latex, fragrances, preservatives and metals. The test can be used to detect allergic reactions that take several days to develop. Allergens are applied to patches and then placed on your skin, either on your arm or back for 48 hours. Irritated skin at the patch site may indicate an allergy.
Foods to avoid with eczema
There is no clear link that has been found between eczema and food allergies. Some people who have eczema are also diagnosed with food allergies and therefore must avoid certain foods to prevent causing or worsening dermatitis.
Some of the foods that people are commonly allergic to that may result in eczema flare-ups include eggs, milk, soy and wheat.
When do you see a doctor?
See a dermatologist if you:
- are so uncomfortable that the condition is affecting sleep and daily activities
- continue to experience symptoms despite trying home remedies
- have a fever or generally unwell together with the rash
- have persistent or worsening skin rashes, especially with wet weepy wounds developing on the skin
If you currently suffer from eczema, don't be disheartened. Consult your dermatologist early and begin taking steps to manage the condition.