The threat of dengue is always present, and while the number of cases in 2023 are far from the surge witnessed in 2022, the National Environment Agency (NEA) remains vigilant as the number of reported cases continues to climb, standing at 7,670 as of the 40th Epidemiological Week.
Besides doing our best to avoid getting bitten by mosquitos and limiting their breeding opportunities in or near our homes, we should also understand the threat the disease poses to our health.
What is dengue?
Dengue is a mosquito-borne disease caused by 1 of 4 dengue viruses, which are transmitted by the female Aedes aegypti or Aedes albopictus mosquitoes.
Symptoms of a dengue infection typically show up 4 – 7 days after being bitten by an infected mosquito. In some cases, dengue may be asymptomatic or present with a mild fever. In more severe cases, patients can suffer from life-threatening dengue shock syndrome. Various factors (such as viral, host, and vector factors) are believed to affect an individual's risk of infection, disease, and disease severity.
What are DenV-3 and DenV-4?
DenV-3 and DenV-4 are less common strains of dengue recorded in Singapore’s history, compared to the more dominant DenV-1 and DenV-2. According to the NEA, DenV-3 has not been prevalent since about three decades ago, and the incidence of DenV-4 has been consistently low. However, in 2021, Singapore saw the first DenV-3 outbreak in 40 years, and a four-fold spike in DenV-4 cases. Collectively, they accounted for more than half of the dengue cases sampled since February 2021. This is a cause for concern, as low immunity among the population towards these two strains leaves more people vulnerable to infection.
Symptoms, and when to consult a doctor
The symptoms for all four strains of dengue are similar, but the community’s response and immunity to each strain may differ. For example, some of us in Singapore may have some form of herd immunity against the DenV-1 and DenV-2 strains, but are more vulnerable against DenV-3 and DenV-4.
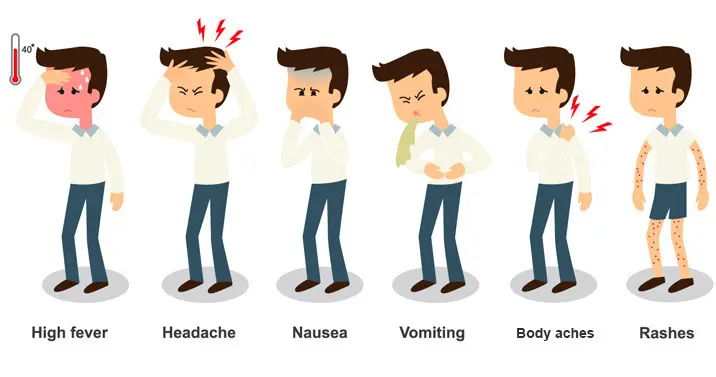
Symptoms of dengue fever typically appear around 4 – 7 days after being bitten by an infected mosquito. It's important to be aware of these 7 warning signs of dengue fever, especially if you reside in an area prone to this mosquito-borne illness:
- Sudden onset of fever: Dengue fever often starts with a sudden and high fever that can last for 2 – 7 days.
- Severe headache with discomfort behind the eyes: Headaches during dengue can be severe and accompanied by pain behind the eyes.
- Joint and muscle pain: Individuals with dengue fever usually experience joint and muscle pain, often described as "breakbone fever."
- Feeling sick and vomiting: Nausea and vomiting are common symptoms of dengue fever.
- Mild bleeding: Dengue fever can lead to minor bleeding tendencies, such as nosebleeds or bleeding gums.
- Skin rashes: Skin rashes are a typical feature of dengue, and they can appear a few days after the onset of fever.
- Fatigue: Dengue fever can leave individuals feeling tired, even after the fever subsides.
It's important to note that in severe cases, dengue fever can progress to dengue haemorrhagic fever or dengue shock syndrome. Severe dengue develops when your blood vessels become damaged and the number of clot-forming cells (platelets) in the bloodstream drops. This is a medical emergency as it can lead to shock, internal bleeding, organ failure, or even death.
Be alert for signs of severe dengue fever which include:
- Severe abdominal pain
- Persistent vomiting
- Bleeding from nose or gums
- Blood in vomit and/or stools
- Rapid breathing
- Fatigue or restlessness
Consult a doctor immediately if you suspect you have dengue fever.
Can you get dengue more than once?
It is possible to get dengue up to four times in a lifetime as there are 4 serotypes of the dengue virus, which are DenV-1, DenV-2, DenV-3, and DenV-4.
Those who recover from an infection will have lifelong immunity against the specific serotype which infected them. While there is evidence of cross-protection, meaning that you may enjoy some immunity against other strains as well, this is only temporary and disappears over the months following infection.
Do the 4 different dengue fever strains differ in severity and symptoms?
In general, the symptoms of a dengue infection from any of the 4 strains are similar. However, differences in clinical manifestations have been reported. For example, a study in 2012 showed that individuals infected with DENV-3 had a higher prevalence of musculoskeletal and gastrointestinal symptoms such as nausea and vomiting, while individuals infected with DENV-4 had a higher prevalence of respiratory and skin manifestations such as rashes.
Several other studies have also suggested that the risk of dengue haemorrhagic fever (DHF), a more severe form of dengue, is highest with DENV-2.
Will a patient be more seriously ill if he or she gets dengue fever a second, third or fourth time?
Multiple epidemiologic studies have shown that the risk of severe disease is significantly higher during a secondary infection than during a primary infection.
During the first infection, the immune system responds by producing antibodies to fight the virus. In subsequent infections with a different serotype (strain) of the dengue virus, the antibodies from the first infection may not be as effective against the new strain. Instead of preventing infection, these suboptimal antibodies may facilitate the entry of the virus into certain cells, particularly immune cells, through specific receptors. This can result in an increased viral load and trigger a stronger immune response, leading to more severe symptoms and potentially progressing to severe forms of dengue, such as dengue haemorrhagic fever.
How can people avoid getting dengue fever in the first place?
Prevention of dengue infection include mosquito control, personal protective measures and vaccination.
Mosquito control can be done by reducing potential mosquito breeding sites. Mosquitoes prefer stagnant water which can accumulation in many areas, especially during the rainy season.
You should also take steps to protect yourself from bites with the use of mosquito repellents and wearing clothing that covers any exposed skin. Use of mosquito screens and insecticides can also help.
For further protection, individuals aged 9 – 45 years with confirmed previous dengue infection may choose to get vaccinated with Dengvaxia. The vaccine should be taken at least 6 months after the initial dengue infection, and requires 3 doses which are administered 6 months apart. Thus far, data shows that the vaccine confers protection for at least 6 years after the last (third) dose of vaccine.
It is important to note that individuals with no prior episode of dengue infection should not take Dengvaxia because studies have shown that the vaccine is associated with an increased risk of severe disease and hospitalisation in this group.
Precautions and prevention of Dengue
While there is no cure for dengue, it can be prevented. Many of the precautions you can take involve making adjustments to your home and lifestyle.
Safeguard your home against mosquitoes with these tips:
- Apply mosquito repellent, even at home.
- Spray insecticide in dark corners of your home.
- Wear long-sleeved shirts and trousers when outdoors.
- Ensure that all windows and door screens are secure and free of holes.
- Use mosquito nets if sleeping areas are not screened.
- Get rid of stagnant water in or around your home.
- Change water in vases/bowls on alternate days.
- Turn over or cover all water storage containers.
- Remove water from flowerpot plates on alternate days.
- Cover bamboo pole holders when not in use.
Why does the Dengvaxia vaccine only work on people who have had dengue before?
The mechanisms are uncertain, but a plausible hypothesis is that vaccination primes the immune system similarly to natural infection. As such, among those with no history of infection, the response to the first natural infection following vaccination may act as a second infection, which has typically been associated with a higher risk of serious disease.
In individuals with prior infection, the response to the first natural infection following vaccination acts as a third or subsequent infection, and is therefore not associated with a higher risk of serious disease.
Where can I find out more about the Dengvaxia vaccine?
To learn more about the Dengvaxia vaccine for preventing and protecting against dengue fever, visit our website or contact a general practitioner at the nearest Parkway Shenton medical clinic. You may also walk into our dedicated vaccination clinic at Esplanade MRT to confirm the availability of the vaccine.